Vitritis Explained: Symptoms, Diagnosis, and Management
What is Vitritis?
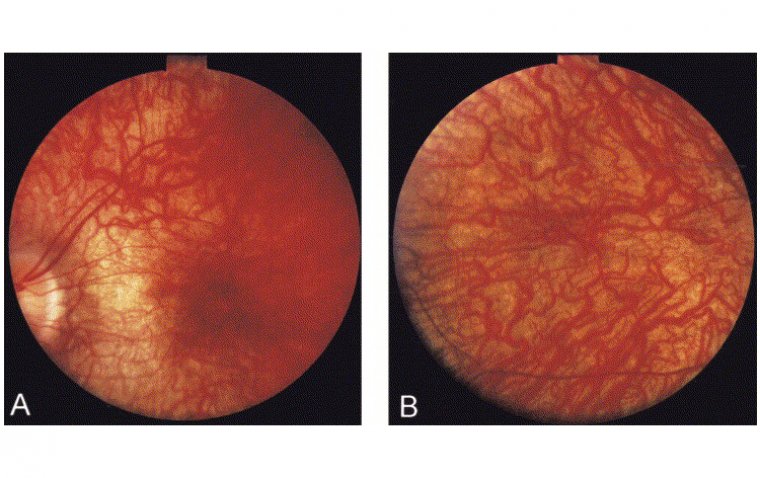
Vitritis is an ocular condition characterized by inflammation of the vitreous, a gel-like substance filling the eyeball behind the lens and in front of the retina. This inflammation can be due to various causes, including infections, autoimmune diseases, or trauma to the eye.
The vitreous plays a crucial role in maintaining the eye's shape and enabling light transmission to the retina for clear vision. Inflammation within this area can lead to a host of visual disturbances and is significant in eye health because it can be a marker for other underlying ocular or systemic conditions. Prompt diagnosis and management of vitritis are essential to preserve vision and address any associated health issues.
What Causes Vitritis?
Vitritis, the inflammation of the vitreous body in the eye, can be triggered by various underlying causes and risk factors. Understanding these is crucial for both prevention and effective treatment:
1. Infections: Various infectious agents, such as viruses, bacteria, fungi, and parasites, can cause vitritis. For example, toxoplasmosis, a parasitic infection, is a common infectious cause of vitritis. Viral infections like herpes simplex and cytomegalovirus, especially in immunocompromised individuals, can also lead to vitritis.
2. Autoimmune Diseases: Systemic autoimmune disorders like sarcoidosis, Behçet's disease, and lupus can cause inflammation throughout the body, including in the eyes. This inflammation can extend to the vitreous, resulting in vitritis.
3. Trauma to the Eye: Physical injury to the eye can lead to inflammation, including in the vitreous.
4. Surgical Procedures: Eye surgeries, particularly those involving the vitreous or retina, can sometimes lead to postoperative inflammation.
5. Idiopathic Causes: In some cases, the exact cause of vitritis remains unknown; this is referred to as idiopathic vitritis.
Signs and Symptoms of Vitritis
Vitritis can manifest through various symptoms, significantly impacting the quality of life and daily activities of affected individuals. Common symptoms include:
● Floaters: These are small, shadowy shapes or specks that drift through the field of vision. In vitritis, the increase in floaters is often a result of inflammatory cells or debris within the vitreous. They can be particularly noticeable against a bright background like a clear sky or a white wall.
● Blurred Vision: Inflammation in the vitreous can interfere with the light passing through the eye to the retina, leading to blurred or distorted vision. This symptom can make it difficult to perform activities requiring sharp visual acuity, such as reading or driving.
● Eye Pain: While not as common as floaters or blurred vision, some individuals with vitritis may experience discomfort or aching in the affected eye.
The impact of these symptoms on daily life can be significant. Floaters and blurred vision can reduce visual clarity, affecting tasks that require precision and attention to detail. This can lead to challenges in professional environments, particularly for those whose work is visually intensive.
Additionally, these symptoms can impair the ability to safely navigate environments, potentially posing risks in activities like driving. Eye pain, although less frequent, can be distressing and may contribute to headaches and discomfort, further disrupting daily routines. The cumulative effect of these symptoms can also lead to psychological stress and anxiety, particularly if the vision impairment is severe or persistent.
How to Diagnose Vitritis
Diagnosing vitritis involves a series of steps and procedures undertaken by eye specialists to accurately identify the condition and its underlying causes. The diagnostic process typically includes:
1. Comprehensive Eye Examination: The initial step is a thorough examination of the eye. An ophthalmologist will review the patient's medical history and symptoms, followed by a detailed examination of the eye. This includes checking for signs of inflammation, assessing visual acuity, and evaluating the health of the eye's internal structures.
2. Slit-Lamp Examination: This is a key diagnostic tool for vitritis. A slit-lamp microscope allows the doctor to examine the structures at the front of the eye under high magnification and can also provide a detailed view of the vitreous and retina to identify any signs of inflammation or debris.
3. Fundus Examination: Using an ophthalmoscope, the doctor examines the back of the eye, including the retina, optic nerve, and blood vessels. This helps in identifying any changes or abnormalities that may be associated with vitritis.
4. Optical Coherence Tomography (OCT): OCT is a non-invasive imaging test that provides detailed cross-sectional images of the retina. It can be particularly useful in identifying any changes or damage to the retinal structures due to vitritis.
5. Fluorescein Angiography: In some cases, this test might be performed. It involves injecting a dye into the bloodstream and taking photographs as the dye passes through the blood vessels in the retina. This can help in identifying any retinal or choroidal vascular problems related to vitritis.Ultrasound of the Eye: If the vitritis is severe and the view of the retina is obscured, an ultrasound may be used to examine the inside of the eye.
6. Laboratory Tests: If an infectious or systemic cause is suspected, blood tests or other laboratory investigations may be conducted to identify specific pathogens or systemic conditions.
Treatment Options for Vitritis
1. Medications: The cornerstone of vitritis treatment is the use of medications. This might include:
● Antibiotics, Antivirals, or Antifungals: If an infection is the root cause of vitritis, specific antimicrobial agents are prescribed to target the infectious organism.
● Corticosteroids: These are commonly used to reduce inflammation in the eye. They can be administered in various forms, such as eye drops, oral medications, or injections directly into or around the eye (periocular or intravitreal injections).
● Immunosuppressive Agents: For cases linked to autoimmune diseases, medications that suppress the immune system might be necessary. These are especially useful in managing chronic or severe inflammation that does not respond adequately to corticosteroids.
2. Laser Therapy or Surgery: In some cases, particularly where there are complications like retinal detachment or severe clouding of the vitreous, surgical interventions may be required. Laser therapy can also be used in certain situations.
3. Monitoring and Follow-up: Regular follow-up appointments are crucial to monitor the response to treatment and adjust the therapy as needed. This may involve repeated eye examinations and imaging tests.
Importance of Early Treatment
Early intervention is vital in managing vitritis effectively. Prompt treatment helps in reducing the risk of complications such as cataracts, glaucoma, or permanent vision loss. It is also crucial for alleviating symptoms quickly, thereby improving the patient's quality of life. In cases where vitritis is a symptom of a systemic condition, early treatment can also help in managing the underlying disease, which is essential for the overall health of the patient.
Prevention and Management
While not all cases of vitritis can be prevented, there are strategies that can help reduce the risk of developing this condition or prevent its recurrence. Additionally, effective management can alleviate its impact on daily life.
Prevention Tips
● Regular Eye Examinations: Routine eye check-ups can help in early detection and treatment of conditions that might lead to vitritis.
● Manage Systemic Conditions: If you have a systemic condition like diabetes, lupus, or HIV, managing it effectively can reduce the risk of associated eye problems, including vitritis.
● Prompt Treatment of Eye Infections: If you develop symptoms of an eye infection, seek prompt medical attention to prevent complications.
● Eye Protection: Protect your eyes from potential trauma, which can be a trigger for vitritis. Use protective eyewear during activities like sports or while working with hazardous materials.
● Healthy Lifestyle: A healthy diet, regular exercise, and avoiding smoking can boost overall health and immunity, potentially reducing the risk of infections that could lead to vitritis.
Managing the Impact on Daily Life
● Follow Treatment Regimens: Adhering to prescribed treatment plans, including medications, is crucial for managing vitritis effectively.
● Regular Monitoring: Keep regular appointments with your ophthalmologist to monitor the condition and make any necessary adjustments to the treatment plan.
● Visual Aids: If vitritis has affected your vision, explore options like magnifying lenses or specialized glasses to help with daily tasks.
● Reduce Eye Strain: Adjusting lighting, taking regular breaks during tasks that strain your eyes, and using anti-glare screens can help reduce discomfort.
● Support Systems: Joining a support group for individuals with eye conditions can provide emotional support and practical tips for dealing with the challenges of vitritis.
● Educate Yourself: Understanding your condition and its treatments can empower you to make informed decisions about your eye health.
Summary
Vitritis is an inflammation of the vitreous humor in the eye, presenting symptoms like floaters, blurred vision, and occasionally eye pain, which can significantly impact daily life. It can be caused by infections, autoimmune diseases, trauma, or surgical procedures, with risk factors including age, immunocompromise, previous eye conditions, and systemic autoimmune disorders. Diagnosis involves comprehensive eye examinations and imaging tests.
Treatment varies based on the underlying cause and may include medications such as antibiotics or corticosteroids, and in some cases, surgery or laser therapy. Early treatment is crucial for effective management. Prevention strategies include regular eye check-ups, managing systemic health conditions, and protecting the eyes from injury. It's important for individuals with symptoms or at risk of vitritis to seek professional healthcare advice for personalized management and to maintain eye health.
(1).jpg)