Iridotomy: Understanding the Procedure, Benefits, and Recovery
What Is Iridotomy?
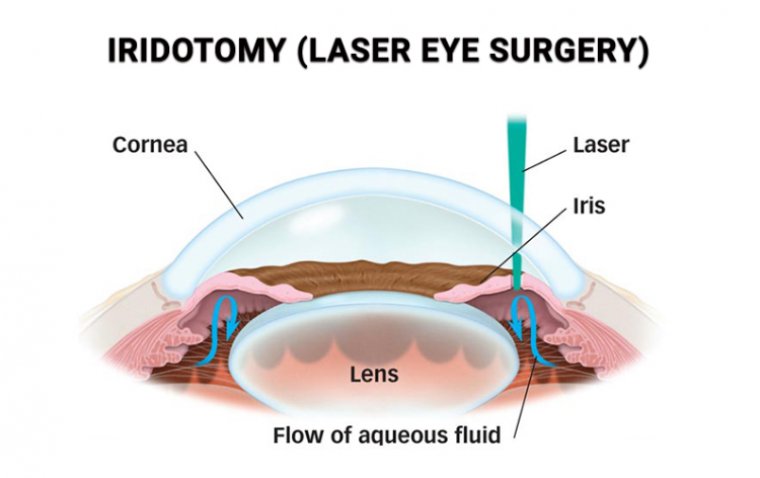
Iridotomy, often referred to as laser iridotomy, is a surgical procedure aimed at treating certain types of glaucoma and other eye conditions that cause an abnormal increase in intraocular pressure (IOP). It involves creating a tiny hole in the iris – the colored part of the eye – to allow fluid to flow freely from the posterior chamber to the anterior chamber of the eye, thereby relieving pressure.
As a minimally invasive procedure, iridotomy is usually performed using a laser and is typically done as an outpatient procedure. Its primary application is in the management of acute angle-closure glaucoma, a condition where the drainage angle of the eye becomes blocked, causing a rapid increase in intraocular pressure. Iridotomy can also be employed prophylactically in individuals identified as being at high risk for this condition.
Understanding iridotomy and its medical applications is crucial, as timely treatment of increased IOP can help prevent vision loss. This surgical procedure is a testament to how advances in ophthalmology can significantly improve patient outcomes in eye health and vision preservation.
Indications for Iridotomy
Iridotomy is primarily indicated for eye conditions that lead to increased intraocular pressure (IOP) due to impaired drainage of aqueous humor, the fluid in the eye. The most common conditions that warrant the need for an iridotomy are angle-closure glaucoma and narrow-angle glaucoma.
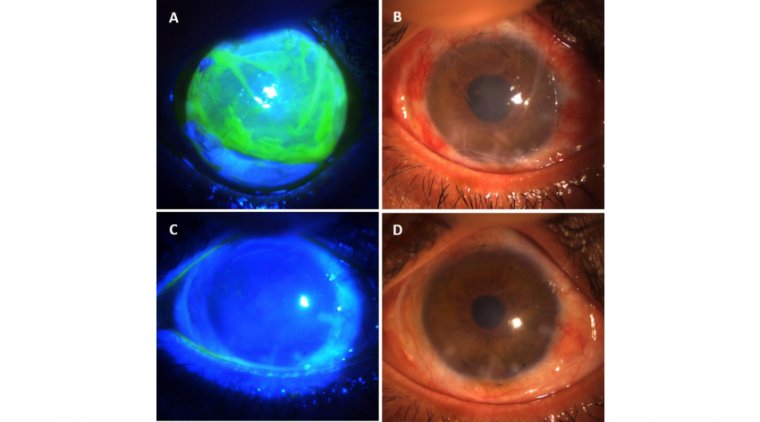
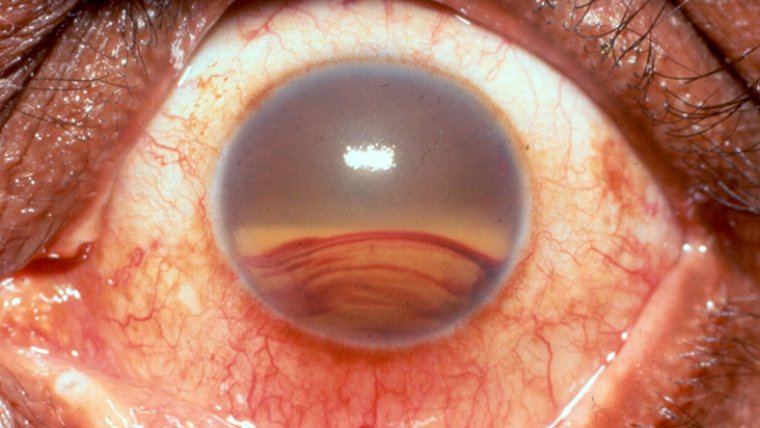
Angle-closure glaucoma, also known as closed-angle glaucoma, occurs when the drainage angle in the eye becomes blocked, typically by the iris. This blockage causes a rapid increase in IOP, which can lead to sudden vision loss if not treated promptly. This form of glaucoma often presents with severe eye pain, nausea, vomiting, and visual disturbances such as halos around lights.
Narrow-angle glaucoma, a subtype of angle-closure glaucoma, is characterized by a narrower-than-normal angle between the iris and cornea. This narrow angle increases the risk of sudden blockage of the drainage system, leading to a rapid rise in IOP.
Apart from these conditions, iridotomy may also be recommended for individuals with anatomically narrow angles, even if they haven't experienced an episode of angle-closure. This is usually determined by an eye care professional during a comprehensive eye examination. The procedure serves as a prophylactic measure, aiming to prevent the occurrence of acute angle-closure glaucoma.
%20(1).jpg)
Benefits of Iridotomy
Iridotomy offers several benefits that make it an effective solution for certain eye conditions, particularly those associated with increased intraocular pressure (IOP).
One of the primary advantages of an iridotomy is its potential to prevent the sudden onset of angle-closure glaucoma. By creating a small hole in the iris, it allows the aqueous humor to bypass the blockage and flow freely, thereby reducing IOP. This can significantly decrease the risk of acute vision loss caused by a rapid rise in pressure.
In cases where the patient already has a diagnosis of angle-closure glaucoma or narrow-angle glaucoma, an iridotomy can stop the progression of the disease and limit further damage to the optic nerve. This is crucial in preserving vision and avoiding the serious complications of untreated glaucoma.
Moreover, iridotomy can help alleviate symptoms associated with increased IOP, such as headaches, eye pain, and blurred vision. By balancing the eye's fluid dynamics, patients often experience improved comfort and reduced ocular strain.
The procedure is also minimally invasive, usually performed with a laser, which means it involves fewer risks compared to more extensive surgical interventions. The recovery period is generally short, and patients can often return to their daily activities soon after the procedure.
Lastly, for patients with anatomically narrow angles, iridotomy serves as a prophylactic or preventive measure, reducing the likelihood of developing acute angle-closure glaucoma in the future. It's a proactive approach in maintaining eye health and safeguarding vision.
The Iridotomy Procedure: Step-by-Step
The iridotomy procedure, while sophisticated, is a relatively quick and straightforward process that can be divided into several key steps:
1. Preparation: Prior to the procedure, an ophthalmologist will perform a comprehensive eye examination to confirm the need for iridotomy. This typically involves measuring intraocular pressure, inspecting the eye's drainage angle, and mapping the patient's visual field. Once the need for iridotomy is confirmed, a date is scheduled for the surgery.
2. Anesthesia: On the day of the procedure, the eye is numbed using topical anesthetic eye drops to ensure patient comfort throughout the surgery. Sometimes, a mild sedative may also be administered to help the patient relax.
3. Eye Dilation: The patient's eye is then dilated with special eye drops. This helps in enlarging the pupil, providing a better view of the iris for the surgeon.
4. Laser Iridotomy: The ophthalmologist uses a highly focused laser to create a small hole in the peripheral part of the iris. The laser energy causes a tiny portion of the iris to vaporize, resulting in a small hole. This allows fluid (aqueous humor) to flow from behind the iris directly to the front, bypassing the pupil, and thus, balancing intraocular pressure.
5. Post-procedure Eye Care: Immediately after the procedure, a steroid or anti-inflammatory eye drop is usually administered to help reduce any inflammation.
6. Monitoring: The intraocular pressure is checked shortly after the procedure to ensure that it is at a safe level. Follow-up visits are scheduled to monitor the patient's recovery and ensure the iridotomy remains open.
Each of these steps contributes to a safe and effective iridotomy, minimizing the risk of complications and ensuring optimal results for the patient's vision.
Preparing for Iridotomy Surgery
Before undergoing an iridotomy, it's crucial for patients to be adequately prepared to ensure the procedure's success and minimize potential complications. Here are the key steps involved in the preoperative preparation:
1. Preoperative Evaluation: The first step towards preparing for an iridotomy is a comprehensive eye exam, which includes tests to measure intraocular pressure and examine the eye's drainage angle. The eye specialist may also carry out a visual field test to map the patient's field of vision.
2. Discussing Medical History: Prior to the procedure, the ophthalmologist will discuss the patient's medical history, including any existing health conditions and current medications. Certain health conditions or medications may affect the surgery, and it's essential to disclose all relevant medical information.
3. Medication Adjustments: Depending on the patient's medical history, some medications may need to be paused or adjusted. For example, patients on blood thinners may be asked to stop taking them temporarily to reduce the risk of bleeding during the procedure.
4. Preoperative Instructions: Before the surgery, the eye care team will provide detailed instructions on how to prepare. This might include refraining from eating or drinking for a certain period before the procedure or using specific eye drops.
5. Arranging Post-Surgery Care: Patients will need someone to drive them home after the procedure, as their vision may be temporarily blurry. It may also be beneficial to have someone at home to help with post-operative care, especially during the initial days following the surgery.
Postoperative Recovery and Care
The recovery period after an iridotomy is an essential phase in ensuring the success of the procedure and the patient's eye health. Here are the key aspects involved in the postoperative recovery and care:
1. Immediate Postoperative Care: After the procedure, the ophthalmologist will typically apply a topical anti-inflammatory eye drop to reduce inflammation. The eye may initially feel gritty or sore, and vision may be blurry. These sensations generally improve within a few hours to a few days.
2. Medications: Patients will usually be prescribed anti-inflammatory and pressure-lowering eye drops to use at home for a week or two following the surgery. These medications help control inflammation and eye pressure, promoting healing.
3. Protecting the Eye: To avoid any complications, patients are advised not to rub their eye and avoid strenuous activities for at least a week. Protective eyewear may also be recommended to shield the eye from injury and bright light.
4. Follow-up Visits: Regular follow-up visits with the ophthalmologist are crucial during the recovery phase. These check-ups allow the doctor to monitor healing and intraocular pressure, ensuring the iridotomy is working as intended.
5. Recognizing Complications: While complications are rare, it's important for patients to know the signs of potential issues. Any sudden increase in pain, loss of vision, or persistent redness should be reported to the eye care professional immediately.
Potential Risks and Complications
While iridotomy is a generally safe procedure, like any surgical intervention, it does carry some potential risks and complications. Here's what you need to know:
● Elevated Eye Pressure: Shortly after the procedure, the intraocular pressure may temporarily rise. This condition is typically managed with pressure-lowering medications.
● Inflammation: The eye might become inflamed following the surgery. This is usually a temporary response and can be treated with anti-inflammatory eye drops prescribed by your ophthalmologist.
● Bleeding: Minor bleeding in the eye can occur during the procedure, which typically resolves on its own without any need for further treatment.
● Vision Changes: Some patients might experience temporary blurring of vision or see an image distortion or glare in their line of sight. These symptoms often improve with time, but it's important to inform your eye doctor if they persist.
● Ineffective Iridotomy: In rare cases, the hole made by the laser could close up, rendering the procedure ineffective. If this happens, the procedure may need to be repeated.
● Infection: Though very rare, any surgical procedure carries a risk of infection. If you experience increased redness, pain, or discharge from your eye, contact your healthcare provider immediately.
Summary
In conclusion, an iridotomy is a crucial surgical procedure designed to treat specific eye conditions, most notably narrow-angle or angle-closure glaucoma. By creating a small opening in the iris, the procedure facilitates the flow of intraocular fluid and aids in the reduction of intraocular pressure, thereby helping prevent serious ocular complications. Preparation for the procedure, understanding the step-by-step surgical process, and adhering to postoperative care guidelines are fundamental for ensuring a successful outcome.
It's also essential to understand that while iridotomy offers significant benefits, like all surgeries, it carries some risk of complications. These are generally rare and manageable, but they underline the importance of professional medical advice and care throughout the process.
The journey to better eye health is an individual one, shaped by unique needs and circumstances. Therefore, anyone considering an iridotomy should engage in in-depth discussions with their eye care specialist, exploring all options and understanding the potential risks and benefits thoroughly. This comprehensive guide is a starting point towards that conversation, and we hope it has given you a clearer understanding of what iridotomy entails.
(1).jpg)