Iris Trauma Repair
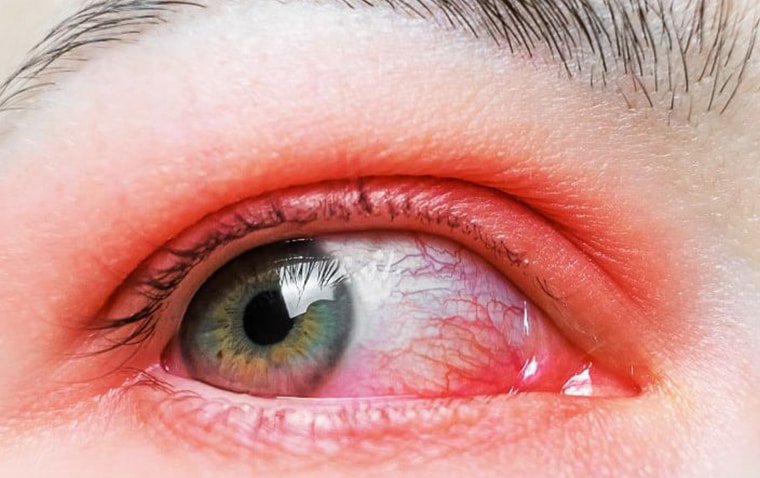
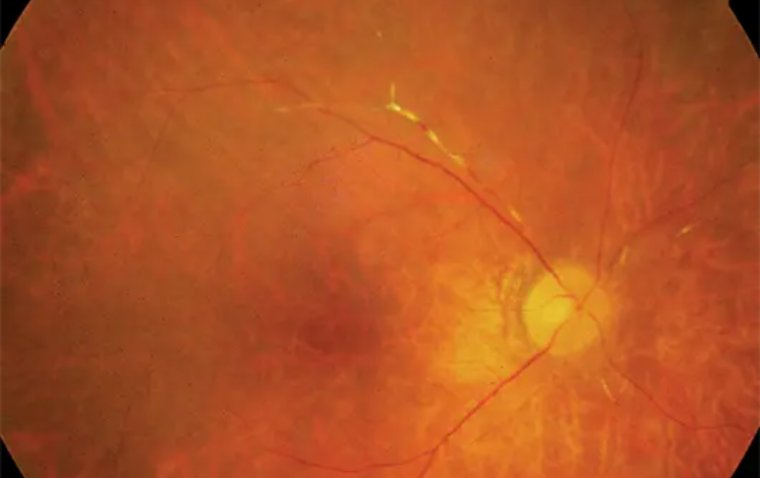
The colorful portion of the eye, the iris, is made up of a ring of muscle and connective tissue fibers that contract and stretch to open and close the pupil in response to the intensity of ambient light.
The iris, which is the colorful portion of the eye that creates the pupil, can occasionally become injured due to trauma or previous surgery.
Patients can occasionally be born with iris abnormalities, and other genetic diseases can even result in the lack of the iris. In these situations, the doctor might suggest to the patient getting some kind of iris surgery. Patients frequently report light sensitivity as a result of too much light exposure, and symptoms of iris disorders are typically secondary to the amount of light that enters the eye.
Patients may also want their eyes repaired for cosmetic reasons if they are self-conscious about how their eyes look. Iridoplasty, or iris repair surgery, and iris prostheses are two types of iris procedures.
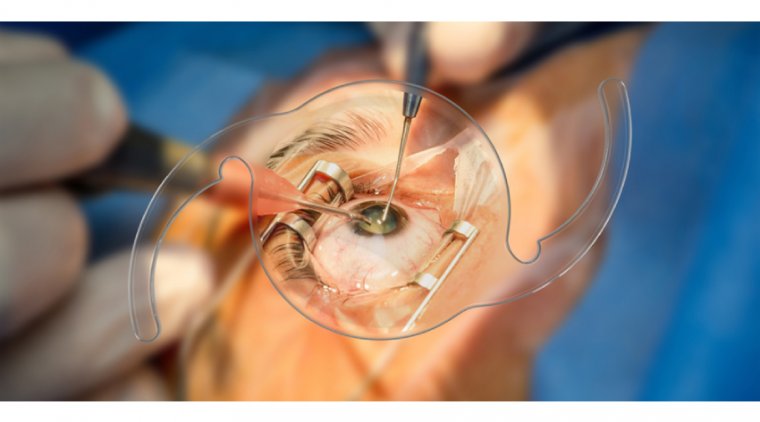
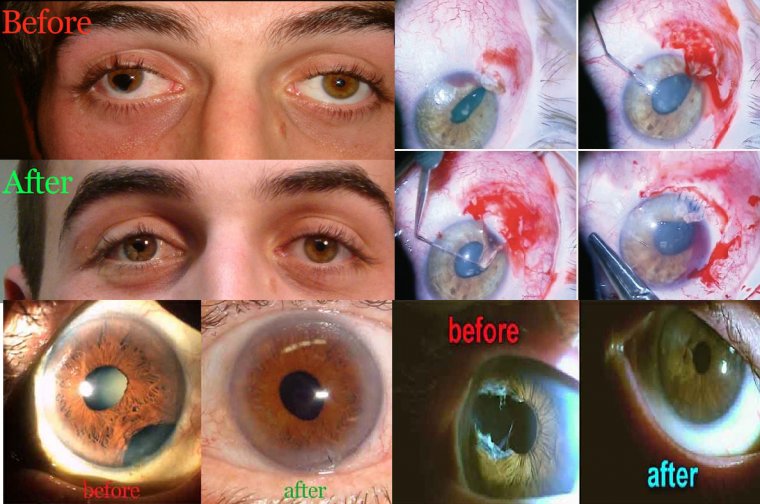
In order to restore the iris to its natural shape and restore a round pupil, iris restoration frequently entails using sutures inside the eye. Sometimes the surgeon will remove a portion of the existing iris to help with aesthetics.
An iris prosthesis can be used if the iris is so severely injured that it cannot be restored. Iris prosthetics entail precisely matching the color of an artificial iris manufactured specifically for the patient to the iris of the opposite eye. The "bag" that houses the lens, also known as the sulcus, is located in front of the artificial iris and can be sutured to the eye's wall (sclera). As an alternative, cataract surgery and the artificial iris placement can be done together.
.jpg)
Reconstructive surgery on the iris is one of the most challenging procedures the anterior segment surgeon performs, especially in cases of ocular injuries.
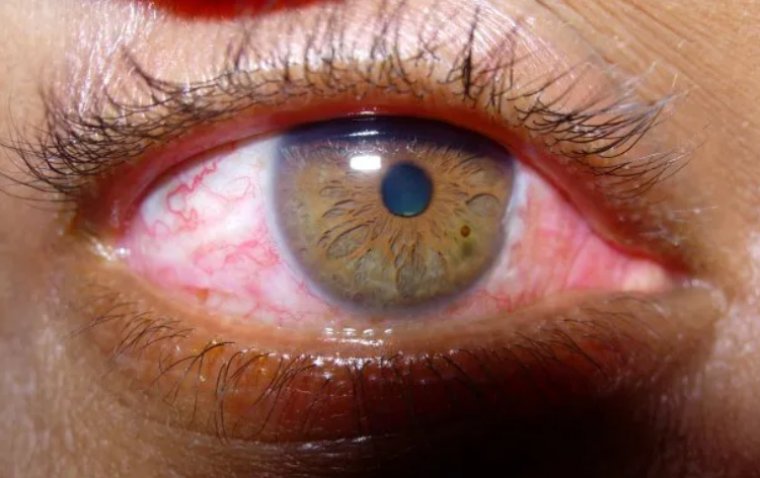
In cases of congenital, traumatic, or other causes of iris loss, patients in need of such reconstructive procedures are frequently severely handicapped by light and glare sensitivity, as well as other visual problems brought on by a damaged iris diaphragm.
Mild to severe visual impairment may exist. Reduced visual acuity and a decrease of contrast sensitivity are further symptoms. Additionally, patients frequently have aesthetic problems, particularly if their iris is light in color. Pupil reconstruction may also be necessary due to abnormalities in pupil size, shape, and placement.
Iris Repair Surgery
Iris repair surgery is a delicate procedure that aims to restore the integrity and function of the iris. The surgery involves using a combination of techniques such as suturing, cutting, and grafting to repair the damaged tissue. The procedure can be done under local or general anesthesia, depending on the extent of the damage and the patient's preference.
The success rate of iris repair surgery is generally high, with most patients experiencing a significant improvement in their vision and quality of life. However, like any surgical procedure, iris repair surgery comes with certain risks such as infection, bleeding, and scarring.
Types of Iris Repair Surgery
There are several types of iris repair surgery, and the choice of procedure depends on the extent and location of the damage. Some of the most common types of iris repair surgery include:
Iris Suturing
This procedure involves using sutures to close any gaps or tears in the iris. The sutures are usually made of a special material that is biocompatible and does not cause any harm to the eye. Iris suturing is a relatively simple procedure that can be done under local anesthesia.
Iris Reconstruction
This procedure involves using tissue from other parts of the eye or a donor to replace the damaged iris tissue. The new tissue is carefully grafted onto the damaged area, and the sutures are used to hold it in place. Iris reconstruction is a more complex procedure that requires general anesthesia.
Iris Prosthetics
This procedure involves using an artificial iris to replace the damaged tissue. The prosthetic iris is custom-made to match the color and size of the patient's natural iris. The prosthetic iris is surgically implanted in the eye and is held in place by sutures. Iris prosthetics is a relatively new procedure that is gaining popularity due to its high success rate and minimal risk of complications.
Iris Prolapse
When there is iris prolapse due to open globe injuries, it is recommended to perform a paracentesis in the opposite direction as the prolapse, followed by the gentle repositioning of the iris using an iris sweep and the injection of a small amount of viscoelastic. Excessive viscoelastic injection can raise pressure and cause more iris prolapse. In these situations, it's crucial to prevent accidentally incarcerating the iris within the suture as well as cutting it, unless it's clearly necrotic or epithelialized, as the iris tissue can be utilised for future reconstruction.
Iris Reconstruction – Traumatic Mydriasis
Globe injuries, whether open or closed, can cause traumatic mydriasis. As an illustration, a case with an iris sphincter tear, a traumatic cataract, and superior iridodialysis—the separation of the iris from its attachment to the ciliary body—are given.
Following trauma, diffuse dilation is another possibility. In these situations, surgical correction may be done concurrently with cataract surgery if the patient is symptomatic. Pupiloplasty with an internal Siepser sliding knot is used for the repair process.
When doing a pupilloplasty, a paracentesis at the limbus is first used to run a 9-0 or 10-0 Prolene suture on a long CTC needle. To make sure no cornea tissue has unintentionally become stuck during the paracentesis, it is crucial to move the needle side to side.
For the purpose of stabilizing the iris for the passage of the suture, MaxGrip forceps can be utilized through a paracentesis. Following that, a loop is externalized through paracentesis, and a Siepser knot is tied. It might be essential to take another bite to close the tiny opening that the second bite created if the iris starts to resemble a keyhole.
Iridodialysis
A tiny, symptomless iridodialysis may occasionally be hidden behind the superior eyelid. Surgery may be necessary for an iridodialysis that is symptomatic and causing diplopia, polycoria, glare, or photophobia.
There are two methods to proceed when surgery is required. In the first scenario, the iridodialysis can be fixed by making a scleral flap; 9-0 or 10-0 Prolene sutures are then threaded through the paracentesis made on the side opposite the iridodialysis site.
Using a 27-gauge needle, the sutures are threaded internally in the eye to dock and externalize them before being knotted beneath the scleral flap. To avoid creating a peritomy, a second strategy is to execute the procedure utilizing a Hoffman pocket.
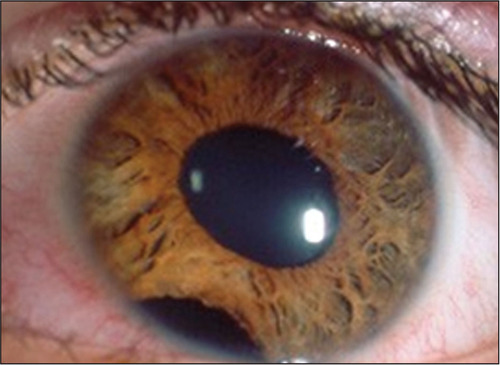
Aniridia
Implantation of an artificial iris (Customflex artificial iris; HumanOptics) may be an option in situations of severe traumatic aniridia. This device's 12.8 mm diameter and 3.35 mm pupil diameter have been approved by the US Food and Drug Administration.
The system is made to match the patient's other eye's color. To guarantee a proper fit in the patient's eye, the device might be trephined. The biggest drawback of the gadget at the moment is that it can be prohibitively expensive and that insurance may not always cover it.
(1).jpg)