Exploring Retinal Vascular Occlusion: Causes and Treatments
Have you ever wondered about the intricate network of blood vessels that sustains our vision? Behind the captivating scenes of our visual perception lies a delicate system vulnerable to a formidable adversary known as retinal vascular occlusion. This menacing condition, also referred to as retinal vein occlusion (RVO), can strike with a swift and stealthy blow, compromising the intricate balance between light and perception.
Central Retinal Vein Occlusion (CRVO) and Branch Retinal Vein Occlusion (BRVO) are the two primary variants of this ocular menace, each capable of casting an indelible shadow on our sight. So, just how serious is retinal vein occlusion, and what can be done to mitigate its impact?
In this article, we will delve into the depths of this insidious ailment, exploring its causes, symptoms, and available treatments. Moreover, we will shed light on the challenges faced by those living with retinal vein occlusion and discuss strategies for leading a fulfilling life despite its presence.
Definition of Retinal Vascular Occlusion
Retinal vascular occlusion, also known as retinal vein occlusion, is a complex condition that affects the delicate blood vessels supplying the retina. It occurs when there is a blockage or obstruction in the retinal veins, impeding the normal flow of blood and nutrients.
Different Types of Retinal Vascular Occlusion
Central Retinal Vein Occlusion
Among the various manifestations of retinal vein occlusion, central retinal vein occlusion (CRVO) stands out as a particularly significant and potentially sight-threatening occurrence.
CRVO occurs when the central retinal vein, a major vessel responsible for draining blood from the retina, becomes obstructed. This blockage disrupts the normal blood flow, leading to a cascade of consequences that can impact vision. The sudden and often dramatic nature of central retinal vein occlusion necessitates prompt medical attention and diligent management to minimize long-term damage.
Branch Retinal Vein Occlusion
Within the realm of retinal vein occlusion, one variant that demands attention is branch retinal vein occlusion (BRVO).
This ocular condition occurs when one of the smaller branches of the retinal vein becomes obstructed, impeding the normal blood flow in that specific area of the retina. Branch retinal vein occlusion can have a profound impact on vision, leading to symptoms such as blurred vision, distorted images, and visual field defects.
Anatomy of Retinal Blood Vessels and Their Role in Occlusion
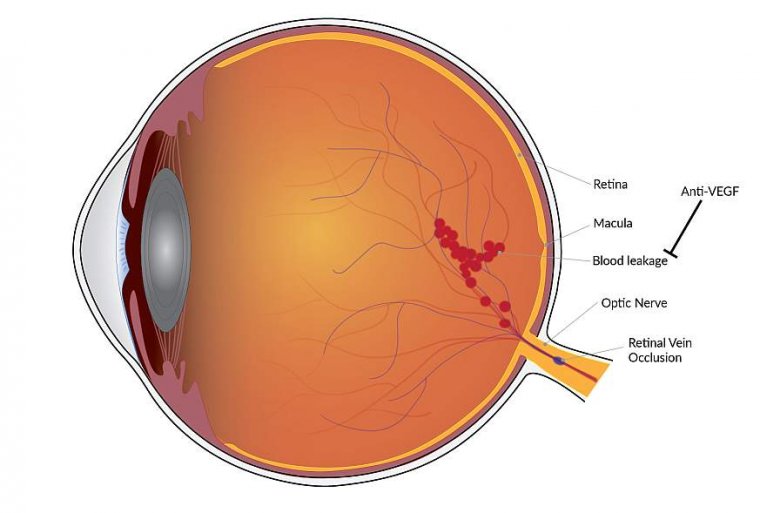
Picture a delicate network of vessels resembling a sprawling tree, nourishing the retina with vital oxygen and nutrients. The retinal arteries bring fresh blood, while the retinal veins carry the used blood away. However, when a hindrance occurs along this essential pathway, the harmony is disrupted. Retinal vein occlusion can arise when these vital vessels encounter blockages or restrictions, jeopardizing the delicate balance between nourishment and vision.
Causes of Retinal Vascular Occlusion
The causes are multifaceted, a complex interplay of various factors that demand our attention. From systemic conditions like hypertension and diabetes that cast a long shadow on the delicate retinal blood vessels, to anatomical abnormalities and clotting disorders that disrupt the harmonious flow of life-sustaining circulation.
Atherosclerosis and Plaque Formation
Within the intricate workings of our circulatory system lies a silent threat known as atherosclerosis, quietly weaving a web of danger that can extend to the delicate retinal blood vessels. This insidious condition, characterized by the formation of fatty deposits called plaque, plays a pivotal role in the development of various cardiovascular complications, including retinal vein occlusion.
The journey begins with injury to the endothelial lining of the blood vessels, triggering a cascade of events. Cholesterol, immune cells, and inflammatory substances gather at the site, leading to the formation of plaque. Over time, this plaque may harden and narrow the blood vessel, impairing the smooth flow of oxygen-rich blood to the retina.
When the retinal veins succumb to the burden of atherosclerotic plaque, the risk of retinal vein occlusion increases. The compromised blood flow can cause swelling, bleeding, and, in severe cases, permanent vision loss.
Embolism and Thrombosis
An embolism occurs when a clot or foreign material, known as an embolus, travels through the bloodstream and becomes lodged in a blood vessel, disrupting the normal flow of blood. This obstruction can impede the nourishing blood supply to the delicate retinal veins, leading to complications.
On the other hand, thrombosis involves the formation of blood clots within a blood vessel, obstructing the flow of blood. These clots, also known as thrombi, can arise from various sources such as damaged blood vessel walls, sluggish blood flow, or conditions that promote clotting disorders.
Common sources of embolism and thrombosis include deep vein thrombosis, atrial fibrillation, atherosclerosis, and certain systemic disorders. Understanding these sources is crucial in recognizing the risk factors and taking proactive steps to prevent their occurrence.
Other Underlying Conditions and Factors
Hypertension is the silent assailant, characterized by persistently high blood pressure, plays a pivotal role in the development of retinal vein occlusion.
The elevated pressure within the arterial walls places undue strain on the fragile retinal veins, making them susceptible to damage and blockages. As the blood vessels struggle to cope with the excessive force, they may become narrowed or even rupture, compromising the essential blood supply to the retina.
Diabetes is the chronic metabolic disorder, characterized by elevated blood sugar levels, exerts a profound influence on the delicate retinal blood vessels.
As diabetes takes its toll on the body, it compromises the integrity of the vascular system, predisposing the retinal veins to damage and blockages. The uncontrolled glucose levels inflict relentless stress on these delicate vessels, impairing their ability to deliver vital nutrients to the retina.
Glaucoma is another factor for developing retinal vein occlusion.
As glaucoma tightens its grip, it disrupts the delicate balance of blood flow to the retina. Increased intraocular pressure impairs the efficiency of blood circulation, compromising the nourishment and oxygen supply to retinal tissues. This compromised vascular environment poses an elevated risk for the occurrence of retinal vein occlusion.
Symptoms of Retinal Vascular Occlusion
| Symptom | Definition |
|---|---|
| Sudden vision loss | Abrupt and rapid decrease in vision, either in a specific area or the entire field of view. |
| Blurred vision | Unclear or hazy vision that may affect the ability to see details and distinguish objects clearly. |
| Distorted images | Visual distortion where straight lines may appear wavy, bent, or crooked, impacting image perception. |
| Darkened curtain effect | The perception of a shadow or darkened area that obscures part or all of the visual field. |
| Floaters | Small, semi-transparent specks, spots, or cobweb-like shapes that drift across the visual field. |
| Flashes of light | The perception of brief, sudden bursts of light that may appear as flickering or lightning-like flashes. |
Diagnostic Tests and Procedures
Healthcare professionals employ a range of specialized tests and procedures to assess the condition and determine the appropriate course of treatment. These diagnostic measures aim to evaluate the extent of retinal vascular occlusion and identify any underlying causes or associated complications.
| Diagnostic Test/Procedure | Description |
|---|---|
| Fluorescein Angiography | Injection of a dye into the bloodstream to visualize the retinal blood vessels |
| Optical Coherence Tomography | Provides high-resolution cross-sectional images of the retina |
| Comprehensive Eye Examination | Assessment of visual acuity, eye movements, pupillary responses, and examination of the eye |
| Visual Field Test | Measures the entire scope of vision, detecting any abnormalities or loss of visual field |
| Intraocular Pressure Measurement | Measures the pressure within the eye to evaluate for potential glaucoma |
| Ultrasound | Uses sound waves to create images of the eye, helping to identify any structural abnormalities |
Treatment Options for Retinal Vascular Occlusion
When it comes to treatment options for retinal vascular occlusion, prompt action is crucial to minimize the risk of permanent vision loss. The approach to treatment involves a combination of immediate management and long-term strategies. In emergency situations, specific emergency measures may be taken.
| Treatment Option | Description |
|---|---|
| Immediate Management | Actions taken in emergency situations to restore blood flow |
| Emergency Measures | Specific measures to address acute occlusion and clot removal |
| Intravenous Thrombolysis | Administering medication to dissolve blood clots |
| Medications | Prescribed drugs to control blood pressure, inflammation, etc. |
| Anti-VEGF Injections | Injections to treat macular edema and promote fluid reabsorption |
| Laser Therapy | Utilizing laser technology to treat abnormal blood vessels |
| Vitrectomy | Surgical procedure to remove the vitreous gel in the eye |
Prevention and Lifestyle Modifications
When it comes to preventing retinal vascular occlusion, adopting a healthy lifestyle is key. Incorporating regular exercise into your routine can improve cardiovascular health, reducing the risk of occlusion. A balanced diet, rich in fruits, vegetables, and omega-3 fatty acids, supports overall vascular health. Avoiding smoking and excessive alcohol consumption further protects against occlusive events. Regular check-ups with your healthcare provider can help identify and manage risk factors for retinal vascular occlusion, such as high blood pressure and diabetes.
Conclusion
Retinal vascular occlusion can occur due to various factors including atherosclerosis, embolism, thrombosis, hypertension, diabetes, and glaucoma. Diagnosing the condition involves visual acuity tests, retinal imaging, and angiography. Treatment options include immediate measures like ocular massage, intravenous thrombolysis, and long-term interventions such as anti-VEGF injections, corticosteroids, and laser therapy. Early intervention and lifestyle modifications are key in managing and preventing retinal vascular occlusion.
(1).jpg)