Management of Mydriasis in Cataract - IOL Surgery
Modern cataract surgery is generally a successful procedure. Recent advancements—which involve the use of pre- and intraoperative pharmacological protocols combined with optimal instrumentation allow for well-tolerated and effective procedures in the vast majority of patients.
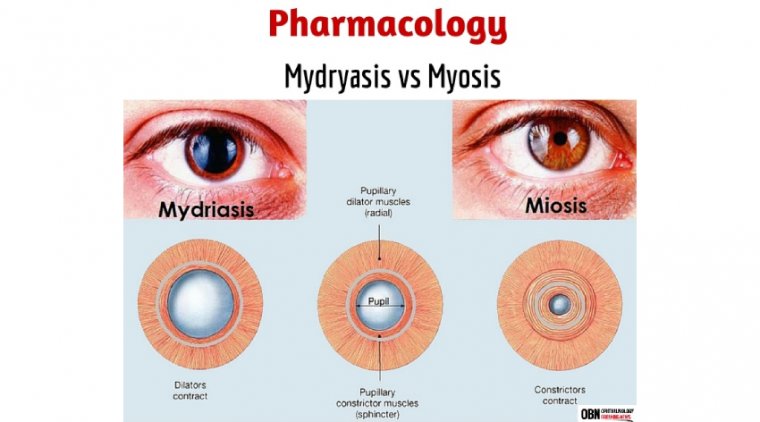
The maintenance of mydriasis and the control of postoperative pain and inflammation are critical to the safety and success of cataract and intraocular lens replacement surgery.
Appropriate mydriasis is usually achieved by topical and/or intracameral administration of anticholinergic agents, sympathomimetic agents, or both, with the most commonly used being cyclopentolate, tropicamide, and phenylephrine.
Ocular inflammation is common after cataract surgery. Topical steroids and nonsteroidal anti-inflammatory drugs are widely used because they have been proved effective to control postsurgical inflammation and decrease pain.
Topical nonsteroidal anti-inflammatory drugs have also been shown to help maintain dilation.
Sufficient mydriasis during cataract removal is critical to a successful surgical outcome. Poor pupil dilation can lead to serious sight-threatening complications that significantly increase the cost of surgery and decrease patients comfort.
Mydriasis is obtained using anticholinergic and sympathomimetic drugs. Phenylephrine, an α1-adrenergic receptor agonist, can efficiently dilate the pupil when administered by intracameral injection.
Additionally, nonsteroidal anti-inflammatory drugs (NSAIDs) like ketorolac, which inhibit the synthesis of prostaglandins, are used to decrease intraoperative miosis, control pain and inflammation associated with cataract surgery, and to prevent the development of cystoid macular edema following surgery.
Modern cataract surgery requires a stable and adequate mydriasis lasting throughout the procedure in order to effectively perform all the steps of the surgery.
The surgeon should assess the quality of dilation during the presurgical examination, and a careful medical history is important to reduce the likelihood of unexpected intraoperative miosis.
Proper mydriasis during cataract removal and IOL placement is critical to achieve a successful surgical outcome by providing a complete visualization of the surgical field, a good red reflex, and adequate room for intraocular manipulation of surgical instruments.
Poor pupil dilation can lead to serious sight-threatening complications such as anterior or posterior capsule tears, vitreous loss and iris trauma during surgery, and the development of cystoid macular edema (CME) or retinal detachment during the postoperative period.
Modern cataract surgery is a generally successful procedure. Recent advances—which involve the use of pre- and intraoperative pharmacological protocols combined with optimal instrumentation—allow for well tolerated and effective cataract surgery in most patients.
However, certain preoperative factors increase the likelihood of complications in cataract surgery. These need to be managed effectively if we want the capsule to remain intact at the completion of surgery.
The small pupil presents one such challenging case for the surgeon. Several techniques have been described in the literature for the management of insufficient mydriasis combined with zonular pathology, ranging from pharmacological to surgical strategies involving mechanical pupil dilation.
To avoid complications, it is essential to enlarge the pupil while also stabilizing the capsule to maintain its integrity. When dealing with patients who present with inadequate mydriasis as well as compromised zonules, we have come to rely on the Malyugin Ring (MicroSurgical Technology [MST]) together with MST Capsule Retractors, Chang Modification.
We find the capsule retractors to be useful in overcoming zonular weakness and giving support to the equator of the capsular bag. However, in some cases, it is possible to use Malyugin Ring 2.0 to address the small pupil and stabilize the capsular bag.
Case Study
The case involves a 75-year-old patient with a cataract complicated by pseudoexfoliation syndrome suboptimally dilated pupil. The patient has been taking tamsulosin for several years to treat benign prostate hyperplasia.
Because the patient’s zonules were loose and the lens was mobile during the capsulorhexis procedure, our strategy was to use the Malyugin Ring 2.0 to address the small pupil and stabilize the capsular bag.
To perform the continuous curvilinear capsulorhexis, we used the 23G Seibel Capsulorhexis Forceps (MST), which feature a sharp tip and a rhexis ruler to allow for visibility and control during the procedure.
In many cases associated with a weak zonular apparatus, the lack of countertraction on the capsule could unintentionally result in a smaller rhexis diameter. A smaller rhexis may not only increase the risk of damage to the capsular edge during the procedure, but also may also cause capsular phimosis in the postoperative period.
Our approach was to use the Malyugin Ring to stabilize the capsular bag and dilate the pupil, so we enlarged the rhexis to prevent the damage to the capsule that may occur while engaging the scrolls of the Malyugin Ring with the capsular edge.
The lens nucleus was fixed with the chopper to avoid excessive movement. A 7.0 mm Malyugin Ring 2.0 was inserted into the anterior chamber. We engaged the iris to support and enlarge it while simultaneously catching the edge of the anterior capsule with the scrolls of the device.
This was done bimanually with the Malyugin Ring manipulator in one hand and the micro-hook retracting the capsular edge in the other hand. In these cases, you only need up to 3 scrolls for the fixation because if you try to use 4, there might be too much stress on the capsule.
Since we were using only the Malyugin Ring 2.0, we did not have the same stability to the capsular bag equator as with the capsular hooks. Therefore, the area with the loose zonules needed to be carefully monitored.
One option is to continuously inflate the capsular bag with dispersive ophthalmic viscosurgical devices to create a viscoelastic cushion and prevent the aspiration of the capsule equator.
We then inserted the conventional capsular tension ring and was able to safely remove the last fragments of the lens by stabilizing the capsular bag equator.
After removing the cortical material, we disengaged the scrolls of the Malyugin Ring from the rhexis and repositioned them to the iris to maintain pupil dilation. When the anterior capsule was released, we could implant a single-piece IOL in the capsular bag.
Finally, the ring was removed from the eye, and triamcinolone acetonide suspension was injected into the anterior chamber to check for the possible presence of the vitreous strands.
Surgeons need to carefully evaluate multiple factors, such as pupil size, rigidity of the iris, sphincter fibrosis, and level of zonular weakness.
The Malyugin Ring 2.0 alone or in combination with capsule retractors helps alleviate complexities in these cases.
For surgeons, it is key to base the choice of instruments for small-pupil cataract surgery on the characteristics of the iris (eg, floppiness or stiffness of the stroma, sphincter fibrosis).
(1).jpg)