Presbyopia & Multifocal Lenses
Bifocal and multifocal contact lenses (CLs) for presbyopia correction and/or myopia control can be made available in a wide variety of platforms, including rigid gas permeable (RGP) lenses of different sizes from corneal to scleral supported, soft contact lenses, and hybrid lenses.
In addition to the lens optical structure, bifocality and multifocality can also be achieved by reshaping the cornea with the application of CLs in the technique called orthokeratology and has been used widely for myopia correction and myopia control although its application for presbyopia correction is still limited.
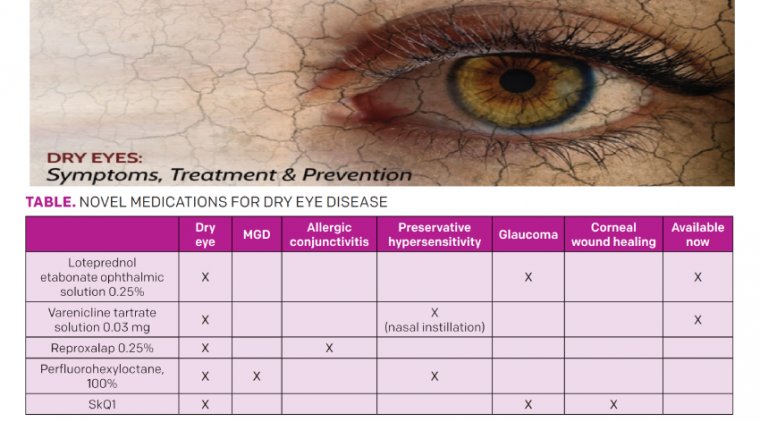
While presbyopia correction with contact lenses accounts for up to 25–35% of the contact lens fittings in several countries, myopia control contact lens fittings are still limited to 2–5% of the contact lenses fitted.
Presbyopia, the gradual loss of accommodation that becomes clinically significant during the fifth decade of life, is a physiologic inevitability.
Different technologies are being pursued to achieve surgical correction of this disability; however, a number of limitations have prevented widespread acceptance of surgical presbyopia correction, such as optical and visual distortion, induced corneal ectasia, haze, anisometropy with monovision, regression of effect, decline in uncorrected distance vision, and the inherent risks with invasive techniques, limiting the development of an ideal solution.
The correction of the presbyopia and the restoration of accommodation are considered the final frontier of refractive surgery. The purpose of this paper is to provide an update about current procedures available for presbyopia correction, their advantages, and disadvantages.
The use of multifocal lenses is a definitive solution in the treatment of presbyopia. Lens implants are the most advanced solution in terms of design and technology since this prevents the need for glasses and allows you to focus at all distances.
Some people decide to have surgery to achieve monovision. This can reduce their need for glasses for near and far objects. Using a laser, an ophthalmologist reshapes the cornea for clear far vision in one eye and close-up vision in the other. In many ways, this is like wearing monovision contact lenses.
The use of scleral contact lenses has grown significantly in the past year with an associated increase in research. This type of lens can be classified as corneo-scleral or fully scleral depending on the presence or absence of corneal bearing.
One of the main advantages of this option for refractive correction is that the tear reservoir between the posterior surface of the contact lens and the anterior corneal surface allows a significant neutralization of anterior corneal aberrations, which are relevant considering the contribution of this optical surface to the total power of the eye.
Because these lenses are fitted with minimal or no corneal bear, the fitting process can be simplified in patients with highly irregular anterior corneal profiles. For this reason, the use of these contact lenses has been intensively investigated for the correction of irregular astigmatism in post-corneal refractive surgery, and post keratoplasty corneas as well as in ectatic corneal disorders.
Although there is a consensus among practitioners with more than 5 years of scleral lens experience about most aspects of contact lens management, some factors require more research, such as the management of multifocality for presbyopia correction.
To date, only the outcomes of conventional soft or rigid gas permeable corneal contact lenses have been evaluated, despite the availability of some multifocal scleral contact lens designs.
Recently, a new model of multifocal corneo-scleral contact lens has been commercially released, called Presbycustom, which provides the option of customizing not only the fitting parameters to adjust the lens over the cornea and sclera, but also the type of multifocality induced.
What follows are the results obtained with this new modality of contact lens in eyes with previous refractive surgery and significant high-order corneal aberrations.
Contact Lens Design
The Presbycustom contact lens (paflufocon D, Dk 100 Fatt units) is the result of a proof-of-concept research project developed by Laboratorios Lenticon SA in collaboration with the Group of Optics and Visual Perception of the University of Alicante in Spain.
It is a corneo-scleral contact lens made of highly gas-permeable material. The lens is customized according to the anterior corneal geometry, the level of ocular high-order aberrations, and the peculiarities of pupil dynamics.
It comprises 3 different areas: corneal, limbal, and scleral (Figure 1). The corneal area has a variable diameter with fixed back-surface asphericity and central anterior surface asphericity that is modified according to the aberrometric induction required. Specifically, the depth of focus achieved with the contact lens is set by customizing the induction of primary and secondary spherical aberration.
It has been demonstrated that combining primary and secondary spherical aberrations of opposite sign is significantly more effective for expanding the depth of focus than other aberrometric options.
The scleral area of the contact lens allows a smooth bearing over the sclero-conjunctival surface, facilitating comfortable wearing (Figure 2). The distribution of the tear film below the different areas of the contact lens generates a characteristic fluorogram consisting of central tear pooling with paracentral alignment and significant edge clearing (Figure 3).
Preliminary Clinical Experience
There has been recently conducted a prospective pilot study in the Department of Ophthalmology of the Vithas Medimar International Hospital in Alicante, Spain, and in the Optometry Clinic of the University of Alicante.
The study included 8 eyes of 8 patients (age 45 to 56 years) with previous LASIK surgery requiring presbyopia correction. All cases had reduced corrected distance visual acuity (CDVA) and significant corneal irregularity.
A complete ocular examination was performed before and 1 month after fitting the customized multifocal scleral contract lens, including visual and refractive analysis, corneal topography, pachymetry and evaluation of corneal and ocular aberrations with the VX120 multidiagnostic system (Luneau Technology, Inc).
The contact lens was customized according to the anterior corneal geometry, level of ocular higher-order aberrations and pupil diameter. The mean corneal radius of the lens fitted was 8.06 ± 0.47 mm; the mean scleral radius was 7.68 ± 0.20 mm.
The mean central eccentricity used for the lenses was 0.44 ± 0.33, whereas a fixed posterior eccentricity of 0.63 was used in all contact lenses fitted. Mean monocular logMAR CDVA changed from 0.21 ± 0.08 with spectacles before fitting to 0.08 ± 0.08 with the contact lens fitted (P=.04).
Mean logMAR binocular distance and near visual acuity values with the contact lens were 0.02 ± 0.03 and 0.14 ± 0.11, respectively. Mean logMAR-corrected visual acuities for defocus levels of -0.50 D, -1.00 D, -1.50 D, -2.00 D, and -2.50 D were 0.03 ± 0.06, 0.08 ± 0.08, 0.19 ± 0.17, 0.24 ± 0.10 and 0.31 ± 0.12, respectively (Figure 4).
All patients reported spectacle independence for reading and high levels of contact lens tolerance and satisfaction. No complications were reported during the first year of follow-up.
The selection of an appropriate combination of primary and secondary spherical aberration of opposite sign according to the aberrometric status of the eye can be useful to optimize the depth of focus required for presbyopia correction.